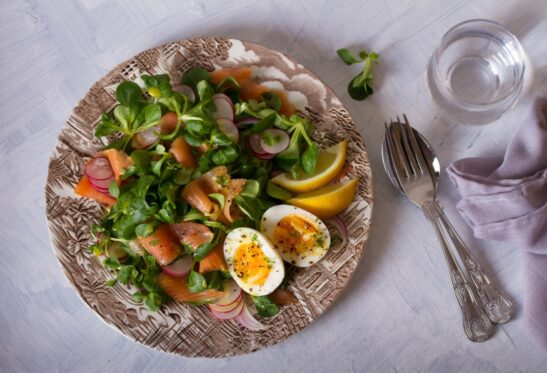Can You Eat Away Allergies? Histamine Intolerance and the Low-Histamine Diet
By Karla WalshHome » Eat Empowered » Can You Eat Away Allergies? Histamine Intolerance and the Low-Histamine Diet
It seems like almost all of us are suffering from some type of food intolerance—or allergy—these days. But if you’ve explored both avenues thoroughly and still haven’t found the culprit for your bloating, constipation, headache or hives even, then you might look into the possibility of something called “histamine intolerance.” You also should get to know how a low-histamine diet might help to treat it.
Below we share the science behind histamines, why some people are intolerant, plus how food (go figure!) plays a role in our relationship with these fascinating chemicals.
What Are Histamines, Exactly?
When you hear “antihistamine” you probably think of an over-the-counter allergy medication. But the body actually makes its own histamines; clearly a sign that they can’t be all that bad for us.
Histamines are chemical messengers that are manufactured within our immune system cells, and are also found in certain foods we eat. Histamines act like guards, protecting the body from foreign invaders and getting rid of something foreign that’s bothering you (AKA an allergen). They’re the memo that tells our bodies to trigger an itchy sensation, a runny nose, watery eyes—whatever is necessary to get said allergen out of our system. They also communicate with the brain to trigger stomach acids to aid in digestion.
Under normal circumstances, histamines are very good at playing defense. But when we have allergies, these histamines can easily overreact to typically harmless things, such as pollen or pet dander. This is when a doctor might recommend an antihistamine medication to tell our innate histamines to chill out.
RELATED: Doctor-Approved Ways to Fight Allergies Naturally
Histamine Intolerance 101
As much as it sounds like “histamine intolerance” might be an intolerance or sensitivity to the actual histamine, this condition actually refers to how our body reacts when it’s exposed to too much histamine.
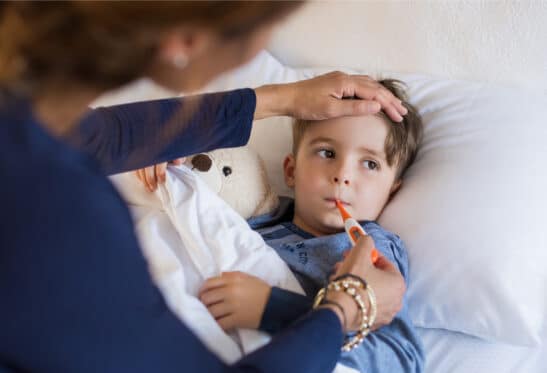
A histamine intolerance can look—and feel—a lot like seasonal allergies, so it can be hard to tell them apart. If you eat histamine-rich foods, you might get the sniffles, watery eyes, and itchy or flushed skin. But some of the more severe symptoms of histamine intolerance might clue you in that it’s not just your seasonal allergies this time. These symptoms can include anxiety or panic attacks, heart palpitations, a full-blown asthma attack, menstrual cycle irregularities or a drop in blood pressure.
It’s estimated that about 1% of people have histamine intolerance, though that’s “a percentage that will possibly increase as more knowledge and diagnostic tools for histamine intolerance become available,” according to recent research.
Histamine intolerance can be genetic or triggered by another medical condition. It’s usually related to abnormal levels of the enzyme diamine oxidase (DAO). When our bodies pump out histamines, we also make DAO, which helps break down the extra histamines in the body and the histamines that we consume via foods and drinks.
DAO deficiencies, often caused by one of the following things, can lead to a histamine intolerance:
- Gastrointestinal (GI) disorders like Crohn’s disease, leaky gut syndrome, acid reflux or inflammatory bowel disease
- Liver conditions
- An unhealthy gut microbiome
- Chronic or severe stress
- Medications (some antibiotics, antidepressants, pain meds and GI drugs) may block DAO production
In addition, as many as 17% of Americans suffer from mast cell activation syndrome (MCAS). Since its symptoms overlap with many other conditions, it often goes undiagnosed. Those with MCAS experience heightened allergy symptoms because mast cells release too often and too much. (Mast cells, which are part of the immune system, release substances called “mediators” when exposed to an allergen.) This results in inflammation, irritation, stomach discomfort, heart rate changes, headaches and more. Since these reactions are in response to histamine exposure, this population in particular may benefit from trying a low-histamine diet. A low-FODMAP diet has also been shown to be helpful for some individuals with MCAs.
RELATED: Could the Low-FODMAP Diet Transform Your Digestion?
What is a Low-Histamine Diet?
Although we wish for—and scientists hunt to find—a definitive answer and a quick Rx, there’s yet to be a proven skin prick or blood test that can diagnose histamine intolerance. Since that’s the case, your doctor may recommend an elimination diet to try to discover if excess histamine is the cause of your symptoms.
It’s tough to quantify exactly how much histamine is in a specific food or drink. Levels within the same type of food—cheese, for instance—can differ widely based on the additives it might include or how long it was aged.
As a general rule, unprocessed foods tend to be low-histamine foods, while fermented foods and alcohol are high-histamine. For more details, read our post on low-histamine foods.
RELATED: This Low-Histamine Food List Might Help Ease Your Allergies
There’s no such thing as a histamine-free diet, but cooking at home rather than eating at a restaurant or ordering takeout can help you more easily control your histamine consumption.
Worth noting: Histamine intolerance isn’t just treated through diet; addressing the gut microbiome, adjusting medications and reducing stress may also help move the needle.
The Bottom Line
Since low-histamine diets are essentially elimination diets, they can err on the restrictive side and don’t work for everyone who has histamine intolerance. It should be considered a short-term “trial,” during which you work with your dietitian and physician to embark on a reintroduction phase.
Just remember, it takes about three to four weeks for histamines to clear out of your body’s tissue, so you want to totally eliminate high-histamine foods from your diet for at least 21 days. Then, slowly reintroduce a single food at a time, taking note of any that lead to worsening symptoms.
(Image: Shutterstock)
Health, Food, Wine and Relationship Writer + Cooking and Wine Event Host
RECENT ARTICLES
Want a sneak peek inside the program?
Get FREE access to some of the core training materials that make up our signature program – Become a Nutrition Coach.
Get Access"*" indicates required fields
 Eat Empowered
Eat Empowered