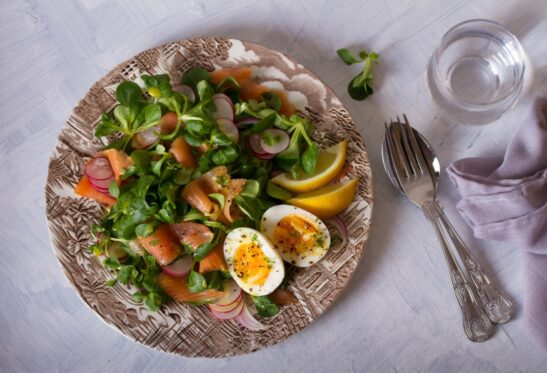Home » Coach » Nutrition Matters: From Bump to Baby – and Beyond
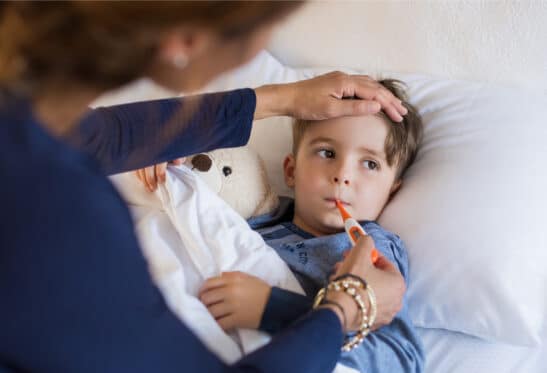
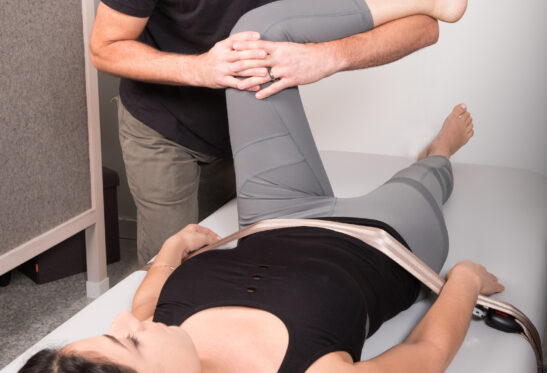
Healthy nutrition is an important part of all stages of a woman’s life, especially during pregnancy and the postnatal phase as both mom and baby are affected. It’s amazing what the body is programmed to do naturally—from conception through breastfeeding. Nutrition is an essential tool when it comes to supporting these processes.
By providing insight into some key pillars of nutrition throughout this part of the life cycle, we as practitioners can facilitate a healthier and more comfortable pregnancy and build a better foundation for wellness after delivery.
Pregnancy and Weight Gain
You may have heard the term “eating for two”. While weight gain is an important part of a healthy pregnancy, a pregnant woman should not actually double her calorie intake. Instead, she should stick to about 300 extra calories a day.
It is important to provide guided counseling around this topic so that the baby can grow at a healthy rate. Gaining too little or too much weight can negatively impact the baby and lead to complications. These include preeclampsia and delivering a baby that is small or large for gestational age.
There are two points to address when talking about weight gain:
1. Optimal Weight Gain Depends on Pre-Pregnancy BMI
If your client was at a healthy weight before pregnancy, aiming to get in 300 extra calories a day is a good target. This could be as simple as adding in an extra nutrient-dense snack or two throughout the day.
Examples of healthful snacks include an apple with 2-3 tablespoons of peanut butter, Greek yogurt with berries, or 1/4 cup hummus with carrots.
An example of a 300-calorie small meal might be avocado toast. If made with a slice of whole-grain bread, one-third of an avocado, one large fried egg and 2 tablespoons of sliced radishes, it clocks in at about 260 calories, according to Food Network.
The actual amount of weight gain that’s considered healthy over the course of a pregnancy depends on an individual’s BMI (body mass index) category, defined below:
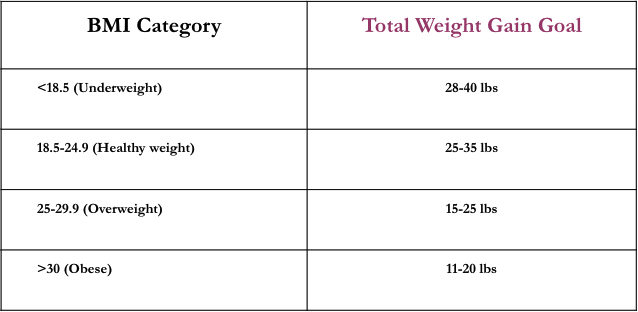
(Source: Institute of Medicine)
2. Nutrient Quality Matters
These extra calories should be coming from nutrient-dense, whole foods with an emphasis on protein for the addition of amino acids, the building blocks of fetal tissue. Fruits, vegetables and whole grains will also provide the valuable vitamins and minerals needed for a healthy baby.
Key Nutrients During Pregnancy
Prenatal vitamins are a great form of insurance to make sure mom and baby are getting enough essential nutrients. Speak with your client and their physician to find the right prenatal vitamins for their needs, and fill in any potential nutritional gaps with whole foods.
RELATED: Are Prenatal Vitamins Safe for Men? Experts Explain How to Support the Health of a Father-To-Be
Below is a breakdown of the eight vital vitamins and minerals for pregnancy. Sharing these categories along with some food lists is a great way to emphasize proper balance in your client’s diet during pregnancy.
Calcium
Pregnant women need about 1,000 milligrams of calcium daily, especially during the third trimester when the baby’s skeleton is rapidly developing. Great sources of calcium include milk, cheese, yogurt and sardines. For vegans, sources might include legumes, leafy greens, almonds and seaweed.
Iron
During pregnancy, an estimated daily intake of 27 mg of iron is recommended to help with the health of red blood cells and their ability to deliver oxygen to the baby. Sources include lean red meat, legumes, peas, and iron-fortified cereals.
Vitamin A
Vitamin A is needed for healthy skin, eyesight and bone growth. Carrots, dark leafy greens, and sweet potatoes are good sources. During pregnancy you need about 770 micrograms daily.
B Vitamins (B-6, B-12, Folic Acid)
B6, or pyridoxine, is a water-soluble vitamin that helps to form red blood cells and is key to the metabolism of protein, fat, and carbs. These macronutrients will either be delivered or stored for the baby. You can find vitamin B6 in beef, liver, pork, whole grain cereals and bananas. During pregnancy, you need about 1.9 mg daily.
B-12 also helps to form red blood cells and maintains a healthy nervous system. You can find this vitamin readily in animal products and a few plant-based sources such as nutritional yeast. Good sources include liver, meat, fish, poultry and milk. During pregnancy you need 2.6 micrograms daily.
Folate: It was less than 50 years ago that British researchers discovered how important folic acid is during pregnancy. They found that too little folate is linked to birth defects of the spine (spina bifida) and the brain (anencephaly.) The thing is, it’s critical for folate to be taken in the first few weeks of pregnancy, often before a woman even knows she’s pregnant. That’s why today the FDA requires some foods to be enriched with folate.
You can find folate in green, leafy vegetables, liver, orange juice, legumes (beans, peas, lentils), and nuts. To reduce the risk of neural tube defects, pregnant women should have a daily folate intake of at least 400 micrograms. Some doctors recommend increasing to 600 micrograms, which is difficult to achieve through diet alone.
Vitamin C
During pregnancy, an estimated daily intake of 85 mg of vitamin C is essential for healthy gums, teeth and bones. Vitamin C also aids in the absorption of iron. Good sources include citrus fruit, broccoli, tomatoes, and strawberries.
Vitamin D
Vitamin D and calcium go hand in hand: Vitamin D aids in the absorption of calcium to help build baby’s bones and teeth. Sources include exposure to sunlight, fortified milk, and fatty fish, such as salmon. It is recommended for pregnant women to get in an estimated 600 international units (IUs) daily.
RELATED: Ask Keri: Can You Get Vitamin D Through a Window?
Omega-3s
According to a meta-analysis published in PLOS Medicine, women who took omega-3 supplements during pregnancy and breastfeeding reduced the risk by 31% for childhood allergic reaction to eggs. For nursing mothers, omega-3 fatty acids from fish, such as wild-caught Alaskan salmon, can help support baby’s brain and eye development by increasing the amount of DHA (a type of omega-3) in breast milk. Aside from salmon, good sources of omega-3s include: flax seeds, chia seeds, walnuts and some plant oils.
Probiotics
The same meta-analysis mentioned above found that probiotics taken after the 36th week of pregnancy and in the first months of breastfeeding were associated with a 22% reduction in the risk for eczema in children. During pregnancy, mom will also benefit from the gut (and brain) health powers of a good probiotic.
Make sure to collaborate with your client’s care team before making any suggestions around supplementation.
Postnatal and Postpartum Nutrition

After delivery, prioritizing nutrition may seem like a difficult task for new moms. A postpartum nutrition plan should be a gentle way to nourish mom back to health and rebuild and repair tissue while also ensuring healthy milk production and all its postnatal benefits for baby.
Studies have also found that better nutritional status helps to lower the risk of postpartum depression. This is because nutrient depletion can affect the production of mood-regulating neurotransmitters such as serotonin.
Here are a few nutrition guidelines to highlight:
Variety
Suggest warm, more easily digestible foods that include a variety of nutrients (high-quality protein, healthy fat, colorful vegetables and whole grains). Soups, stews and collagen-rich proteins (beef, bone broth) are great sources of anti-inflammatory nutrients that aid in the rebuilding of tissues and production of breast milk.
Calories
Exclusively breastfeeding women will require about 400 to 500 extra calories per day. (Yes, that’s more than what a woman needs during pregnancy!) Breastfeeding can burn more fat stores, so emphasizing healthy dietary fat from nuts, seeds, avocados and full-fat yogurt is important for these moms.
Hormone Balance
The body will naturally aid in the recalibration of hormones—such as estrogen and progesterone—postpartum, but there are ways to support these processes with nutrition:
- Recommend pairing protein with moderate carbohydrate to keep blood sugar stable
- Eliminate highly processed, packaged foods, and focus on whole foods that are rich in protein, fiber, antioxidants, and healthy fats
- Recommend the continuation of a prenatal vitamin routine for up to a year to help support hormone and vitamin/mineral balance
- Encourage activity/exercise such as walking, yoga, pilates once their doctor has given the OK. This can help regulate cortisol levels, which can be made in excess when you’re not getting enough sleep, a phenomenon that most new moms are very familiar with.
Hydration
Fluids are highly important. For breastfeeding mothers, 10 to 15 glasses of water a day is recommended to quench thirst and produce breast milk. If you need some help drinking this much water, may we suggest infusing your water with fruit like this pineapple water.
Nutrition Matters: From Bump to Baby – and Beyond
Supporting your client’s journey from bump to baby can be such a rewarding process. No matter what stage a mom-to-be may be in, providing tangible wellness tips will not only help with physiological processes but emotional factors as well – for both mom and baby!
With so much emerging research on the fetal microbiome and health outcomes later in life, you are indirectly providing counseling for two!
Become a Master Certified Nutrition and Wellness Coach
Considering a career in pregnancy coaching? Discover how becoming a Nutritious Life Master Certified Nutrition and Wellness Coach can make a difference in your life – and the lives of your clients. The Nutritious Life Studio supports a thriving community of wellness professionals in building and growing their healthy businesses.
(Images: Shutterstock)
Ellie Erlich is a registered dietitian and holds a Master of Science in clinical nutrition from New York University. She is the program mentor for The Nutritious Life Studio and works privately with clients to accomplish a wide range of wellness goals from weight loss to chronic conditions and autoimmune disorders.
RECENT ARTICLES
Want a sneak peek inside the program?
Get FREE access to some of the core training materials that make up our signature program – Become a Nutrition Coach.
Get Access"*" indicates required fields
 Eat Empowered
Eat Empowered